Lisa Simpson “started living again” after she received her nerve stimulator. In July 2007, she took a two-week rafting trip in Alaska.After 15 years of battling fibromyalgia with medication and exercise, Lisa Simpson still had cramping, spasms, and pain all over her body. "Just to have my 7-pound Chihuahua walk over my legs would cause severe pain," the 37-year-old medical assistant recalls.
Simpson had all but given up on finding relief when, in 2004, she saw a ray of hope. She was working in the office of an anesthesiologist at Griffin Hospital in Derby, Conn., Mark Thimineur, MD, who had begun surgically implanting tiny, nerve-stimulating devices into fibromyalgia patients.
"Some of the patients could barely make it from one end of the office to the other," she recalls. After the treatment, "they had a spring in their step" and were "like a totally different person."
The treatment, known as peripheral nerve stimulation (PNS), entails implanting wire electrodes that are about 2 millimeters thick just beneath the skin of the patient's head or lower back. The electrodes, which are connected to a battery-powered stimulator, deliver a mild—and usually imperceptible—electrical current to certain nerves.
Easing the pain of fibromyalgia
- 10 Food Rules for Pain Patients
- Prescription Medications for Fibromyalgia
- 10 Products That Ease the Pain of Fibromyalgia
The technique is commonly used for severe back pain, leg pain, and headaches, but Dr. Thimineur is one of just a handful of doctors who use PNS to treat fibromyalgia, a poorly understood and hard-to-diagnose condition marked by widespread pain and tenderness.
The Food and Drug Administration (FDA) has not approved nerve stimulation for fibromyalgia (or headaches). It's considered an experimental treatment and is used only in people with near-disabling fibromyalgia who have failed to respond to other treatments.
However, up to 40% of the approximately 10 million fibromyalgia patients in the U.S. fall into that category, and if PNS proves beneficial, it could potentially help tens of thousands of people, without the side effects of prescription drugs.
But for that to happen—and for insurance companies to agree to foot the hefty bill (it can cost up to $90,000)—clinical trials will need to prove its safety and efficacy. "This is on the cutting edge, or witchcraft," says Peter Staats, MD, a pain doctor in private practice in Shrewsbury, N.J. "We haven't decided which yet."
The results described by patients can indeed sound too good to be true. Simpson underwent the treatment herself, and she estimates that it halved her fibromyalgia symptoms.
"It was like a light switch," says Simpson, who now helps Dr. Thimineur counsel and monitor patients receiving nerve stimulation. "As soon as the machine was turned on, it was like night and day."
Next Page: A tingling sensation [ pagebreak ]
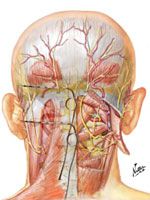 occipital-neuro . (In May, he and several colleagues received a patent for the technique he uses.)
occipital-neuro . (In May, he and several colleagues received a patent for the technique he uses.)
The improvement that Simpson saw is the norm rather than the exception, Dr. Thimineur says. He estimates that between 50% and 60% of his fibromyalgia patients experience a 50% reduction in pain (a common benchmark used to assess pain treatments), qualifying them for an implant.
Mark Plazier, MD, a neurosurgeon and colleague of Dr. De Ridder's at University Hospital Antwerp, in Belgium, says that the overall improvement in a patient's quality of life is even more impressive than the pain reduction. "They just get back into shape, back into society," he says.
The treatment doesn't always go smoothly. Finding the right level of electrical current for each patient is more art than science: Too low, and the pain relief will be negligible; too high, and side effects such as anxiety—and, counterintuitively, headaches—can occur. (If the current is right, side effects are minimal, Dr. Staats says.)
Lori Masters, a 46-year-old mother of four, received the treatment from Dr. Thimineur in 2005 to treat her chronic headaches. Although it didn't help her migraines, Masters says the stimulation "totally obliterated" her fibromyalgia pain, increased her energy, and cleared the mental cloudiness known as "fibro fog." But these benefits came at a price. For the first year, she experienced tingling and irritability because settings on her stimulator were too high.
"I would get jittery and anxious, like I had too much coffee," she says. "I found myself yelling at my kids, which I don't usually do."
Dr. Thimineur decreased the current at each monthly visit, to the point where it was actually too low. Masters lost her jitters and anxiety, but her pain came back, and she felt exhausted. After a small increase, Dr. Thimineur hit upon the right level for her. She has done well ever since and can now attend her daughter's basketball games—something she was in too much pain to do before.
Next Page: The challenges of research [ pagebreak ]
The challenges of research
Joshua Greenspan, MD, a pain specialist in private practice near Portsmouth, N.H., has treated at least 50 fibromyalgia patients with nerve stimulation. But he says more research is needed for doctors to embrace the technique. "There has to be at least one paper with at least 100 people in it," says Dr. Greenspan, who first learned about using nerve stimulation for fibromyalgia from Dr. Thimineur.
In order to demonstrate the treatment's efficacy for fibromyalgia, randomized, placebo-controlled trials will have to rule out the possibility that the placebo effect is responsible for the pain reduction. Designing a placebo (or "sham") version of nerve stimulation can be a challenge, however; because the electrical current often produces a noticeable tingling, it's difficult to "blind" a patient to whether she's receiving the real thing. (The research supporting other nerve-stimulation techniques, such as the treatment known as TENS, has been called into question for this reason.)
Separating the treatment effect from the placebo effect may be especially tricky with fibromyalgia. Compared to, say, back pain, the disorder is relatively difficult to diagnose and often overlaps with other health conditions that contribute to pain symptoms, including lupus, arthritis, and depression.
Dr. Plazier and Dr. De Ridder think they've found a way around the placebo problem. In a recently completed study that included 11 fibromyalgia patients, they dialed back the amount of current such that the patients experienced pain relief but no tingling sensation. Then, over two five-week periods, they compared the effect of this "subthreshold" current to the effect of the wires being off altogether, without the patients knowing which was which.
The preliminary findings—which have not yet been accepted by a peer-reviewed journal—are encouraging, the researchers say, and they are now conducting a similar study with 40 patients that they hope to finish next summer.
Still, it's likely to be several years before nerve stimulation becomes a mainstream treatment for fibromyalgia. "The way we're using peripheral nerve stimulation is more of a paradigm shift," Dr. Thimineur says. "Paradigm shifts occur slowly."
Costs and benefits
Proving that peripheral nerve stimulation is superior to placebo will be necessary in order for insurance companies to agree to pay for the procedure. Currently, some insurance companies—and in some states, Medicaid and Medicare—cover the treatment for chronic headaches and other pain conditions, but not fibromyalgia.
Dr. Greenspan estimates that private insurers would recoup the costs of the treatment in about two years if they decide to cover eligible fibromyalgia patients. Part of the savings would come from medications, which most patients can stop taking after beginning nerve stimulation, Dr. Greenspan says.
Simpson discontinued her regular pain drugs within two months of getting her implant, and now she only takes them to help with brief spells of "breakthrough" pain. As with many nerve-stimulation patients, her pain returns every year or so—a signal that she needs to have her stimulator setting readjusted.
After Simpson's last episode of breakthrough pain, Dr. Thimineur upgraded her stimulator battery and moved the wires slightly higher up in the back of her head, where they have a stronger effect. For the first time in six years, she was current-free for several weeks while Dr. Thimineur evaluated her baseline level of pain.
"I can see all the old pain starting to come back with the stimulator off," says Simpson, who missed more work than she could make up in those weeks. "I don't know how I managed before."
