Atopic dermatitis, also known as eczema, can make the skin all over your body feel dry, red, and itchy. And, unfortunately, your scalp isn't immune to the effects of atopic dermatitis, even though it's covered in hair.
"It's an intrinsic defect of the skin barrier," Dendy Engleman, MD, FAAD, a board-certified dermatologist in New York, tells Health. Essentially, people with eczema have super sensitive skin, and the condition can cause patches of very itchy, red skin that look dry and cracked.
Atopic dermatitis most commonly appears on the arms—specifically the area in front of or inside the elbow—or behind the knees. But you can get it anywhere on your body, says Dr. Engleman, including on your scalp. Here's what you need to know about atopic dermatitis on the scalp, including how it's different from other scalp conditions, how to spot it, and how it's treated.
RELATED: What Is Atopic Dermatitis? (and How to Tell If You Have It)
What is atopic dermatitis on the scalp?
Atopic dermatitis on the scalp is eczema that affects the skin on top of your head. "It's more rare but we do see patients who have [eczema] on their scalp," Emma Guttman-Yasky, MD, PhD, the Waldman professor of dermatology and immunology and system chair department of dermatology at the Icahn School of Medicine at Mount Sinai, tells Health. Patients who have severe eczema on many other parts of their bodies can often get it on their scalp, she says.
However, what people think is scalp eczema is often actually one of two other conditions, she says: seborrheic dermatitis (aka dandruff) or psoriasis. They're often mistaken for each other because they have very similar symptoms—red, itchy, dry patches of skin. But the three conditions are very different. Here's a quick overview:
- Atopic dermatitis: As mentioned, atopic dermatitis is an inflammatory skin disease that causes red rashes to break out over certain parts of the body. Per the American Academy of Dermatology (AAD), it is triggered by a complex mix of genetic and environmental factors. It makes the skin incredibly sensitive, adds Dr. Engleman, and more at risk of infections.
- Psoriasis: a chronic condition that causes itchy, scaly patches on the skin, including the scalp. There are a few different subtypes, but the most common type of psoriasis causes dry raised patches covered in scaly skin. According to the AAD, it's believed to be caused by a faulty immune response, which forces skin cells to grow back faster than normal. (Genetics can also play a role.)
- Seborrheic dermatitis: an inflammatory condition caused by yeast overgrowth on the scalp, the AAD says. It can occur in hair-bearing areas, says Dr. Engelman, including the scalp, eyebrows, and chest. It can cause skin flakes, patches of greasy skin covered with scales or crust, and itching, and is typically treated with antifungal medications.
RELATED: 13 Things That May Make Atopic Dermatitis Worse
What are the symptoms of atopic dermatitis on the scalp—and what does it look like?
Once again, all three conditions—atopic dermatitis, psoriasis (and scalp psoriasis) and seborrheic dermatitis—can all present similarly with itchy, dry patches of skin. Here are some of the symptoms most closely related to atopic dermatitis on the scalp, specifically.
- Extreme itchiness: This is the hallmark of any form of atopic dermatitis, says Dr. Guttman-Yasky. "The patients with eczema on the scalp, they will itch it," to the point of leaving wounds that bleed on their scalp, she adds. "If it doesn't itch, it's unlikely to be eczema."
- Skin flakes: Like seborrheic dermatitis, Dr. Guttman-Yasky says, atopic dermatitis on the scalp can cause skin flaking. This can be due to the dryness of the skin there or from people scratching at the itchy skin for relief.
- Temporary hair loss: This can sometimes happen with scalp eczema, says Dr. Guttman-Yasky. "But usually when we treat them well, [the hair] should come back because the follicles should still be there," she adds.
- Darker red patches: This is a common symptom of atopic dermatitis no matter where it occurs on the body, per the AAD. It might be trickier to spot on your own scalp if covered by lots of hair.
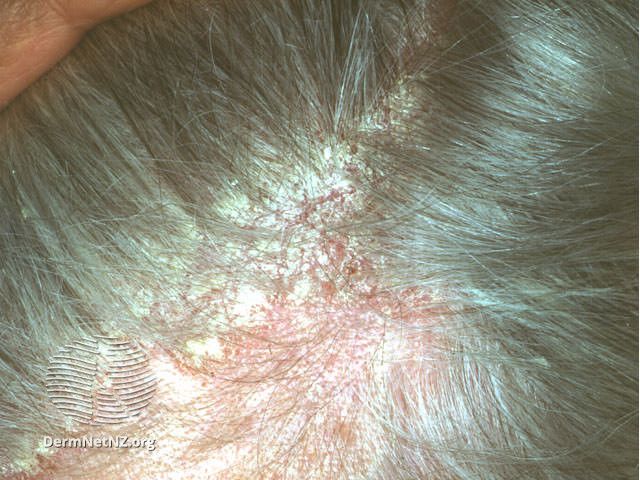 Atopic-Dermatitis-on-Scalp-sebderm6__WatermarkedWyJXYXRlcm1hcmtlZCJd
Atopic-Dermatitis-on-Scalp-sebderm6__WatermarkedWyJXYXRlcm1hcmtlZCJd
What causes atopic dermatitis on the scalp?
Atopic dermatitis is generally a complex condition with a variety of causes and risk factors, says Dr. Engleman. It's often genetically inherited, she says, so if your mom or dad have it, you're more likely to develop it too. Eczema also seems to be influenced by something called the atopic triad, she says—seasonal allergies, asthma, and eczema. (Basically, people with eczema often also have seasonal allergies and/or asthma.) People with eczema also often have genetic mutations that affect how effective their skin barrier is at protecting you from germs, irritants, and other pathogens, she adds.
No matter the cause, the end result is that people with eczema have super sensitive skin that overreacts to things that aren't supposed to be irritating, says Dr. Engleman. In the case of the scalp, the eczema flareup just happens to occur on the scalp. Having an existing flare-up of eczema affecting large parts of your body can potentially eventually involve the scalp, according to Dr. Guttman-Yasky says.
RELATED: This Makeup Artist With Chronic Eczema Doesn't Hide Her Flare-Ups—She Makes Them Stand Out
How can you treat and prevent atopic dermatitis on the scalp?
Because it can easily be confused with other skin conditions, your first order of business if you think you have scalp eczema is to see a board-certified dermatologist. They can properly diagnose you and provide the correct treatment—which will require a prescription.
Dr. Guttman-Yasky says that she typically prescribes a combination of topical steroids (which are potent anti-inflammatories) and salicylic acid (a common skin-care ingredient used to facilitate skin cell growth, unclog pores, and more) for people with true atopic dermatitis on their scalps. This combo helps remove any scaly buildup caused by eczema while combatting itchiness, she says. If a patient's eczema is all over their bodies, not just their head, or is particularly severe, she says she might opt for a systemic course of steroids.
Your dermatologist might also recommend you change some aspects of your hair-care routine to help reduce itching and reduce the risk of future flareups. "We recommend mild shampoos with a minimum amount of preservatives," Dr. Guttman-Yasky says, because those kinds of ingredients can be irritating to sensitive, eczema-prone skin. (Look for brands that say they are preservative-free, or look at the label to make sure it doesn't have parabens, formaldehyde, or formaldehyde-releasing ingredients like DMDM hydantoin.)
People who have or frequently get scalp eczema should also avoid going overboard on hair treatments, like tons of blow drys or regular bleaching, Dr. Guttman-Yasky adds. These treatments are harsh and could unnecessarily irritate a sensitive scalp.
While it may be less common than seborrheic dermatitis or psoriasis, atopic dermatitis on the scalp can still happen—and requires a dermatologist's help. "It's hard to differentiate these [conditions] and you need to go to a specialist," Dr. Guttman-Yasky says. And it's not something you can just treat at home. So if you have unbearable itching on your head (or any other part of your body, for that matter), consider it time to book an appointment with your derm ASAP. Your scalp will thank you for it.
To get our top stories delivered to your inbox, sign up for the Healthy Living newsletter
